The first person in Germany to write an obstetrics book from a woman's perspective, Justine Siegemund made childbirth safer for both mothers and their children.
Childbirth in the 17th century could be a dangerous business. Knowledge about the process was limited, and simple complications could sometimes be fatal for both women and their babies. Justine Siegemund set out to change that.

Public DomainBecause medical books of her day were written by men, Justine Siegemund decided to write an obstetrics book from a woman’s perspective.
Motivated by her own health struggles, Siegemund educated herself on women’s bodies, pregnancy, and childbirth. She not only became a talented midwife who safely delivered thousands of babies, but she also described her techniques in a medical text, The Court Midwife (1690).
Siegemund’s book, the first medical book written in Germany from a woman’s perspective, helped revolutionize childbirth and make it safer for women.
This is her incredible story.
How Personal Health Problems Inspired Justine Siegemund’s Work
Born in 1636 in Rohnstock, Lower Silesia, Justine Siegemund didn’t set out to improve childbirth. Rather, she was motivated to learn more about women’s bodies as a result of her own health struggles.
As an article in the American Journal of Public Health reports, Siegemund had a prolapsed uterus, which meant that the muscles and ligaments around her uterus had weakened. This would have caused symptoms like a feeling of heaviness in Siegemund’s lower abdomen, and many midwives erroneously treated her as if she were pregnant.
Frustrated by their treatment, Siegemund set out to learn about midwifery herself. At the time, childbirth techniques were spread by word of mouth, and midwives often fiercely guarded their secrets. But Siegemund was able to educate herself, and she started delivering children around 1659.
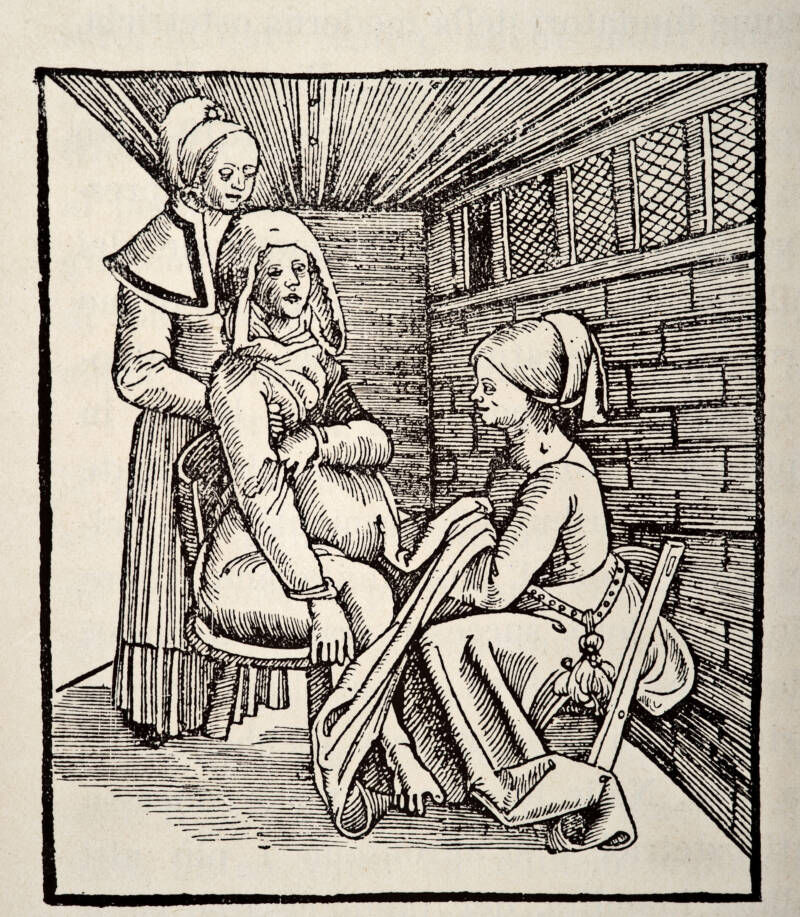
VintageMedStock/Getty ImagesA medical drawing depicting childbirth from Justine Siegemund’s book, The Court Midwife.
Unlike many of her colleagues, Siegemund rarely used drugs or surgical instruments while delivering babies. She initially worked only with poor women, but she quickly made a name for herself, and she was soon called to work with women from noble families as well. Then, in 1701, as word of her talent spread, Justine Siegemund was summoned to Berlin to work as the official court midwife.
Justine Siegemund Writes The Groundbreaking Obstetrics Book, The Court Midwife
As the court midwife in Berlin, Justine Siegemund’s reputation grew rapidly. She delivered babies for the royal family and helped noble women with health problems like cervical tumors. The American Journal of Public Health notes that Queen Mary II of England was so pleased with Siegemund’s work that she asked her to write an instructional text for other midwives.
Though midwifery was largely an oral tradition and medical texts were typically written by men, Siegemund complied. She wrote The Court Midwife in 1690 to share her knowledge with others. She described how she had delivered healthy babies at 37 weeks, dispelling the idea that infants could only survive after 40 weeks, and the importance of puncturing the amniotic sac to prevent “hemorrhage in placenta previa.”
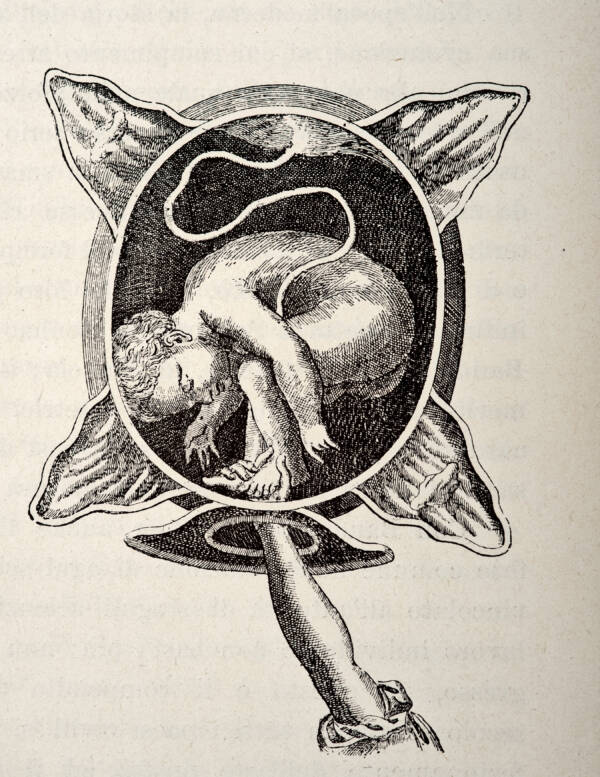
VintageMedStock/Getty ImagesA medical engraving from the The Court Midwife demonstrating a breech delivery.
Siegemund also described how she had guided mothers through difficult births, like when their babies were born shoulder first. At the time, such a birth could be fatal for both woman and child, but Siegemund explained how she was able to rotate the infants to safely deliver them.
By sharing her expertise, Siegemund was also able to push back against the myth that babies could only be delivered by men, according to Indy 100. That said, Siegemund also roused the ire of many male physicians and midwives, who accused her of spreading unsafe birthing practices.
Despite these attacks, Siegemund’s book became the first comprehensive text on childbirth in 17th-century Germany. Before then, there hadn’t been a standardized text that doctors could share to educate themselves about safer childbirth techniques. And it didn’t take long for the The Court Midwife, first published in German, to be translated into other languages.
But perhaps the best testament to Justine Siegemund’s impact on childbirth is her own record. When she died in 1705 at the age of 68, a deacon at her funeral in Berlin made a stunning observation. During her life, Siegemund had successfully delivered almost 6,200 babies.
After reading about Justine Siegemund, go inside the grisly history of symphysiotomy, the childbirth procedure that led to the invention of the chainsaw. Or, learn about the Blonsky Device, which was created to “fling” babies out of women during childbirth.






